You get a diagnosis like osteoporosis, and suddenly your questions get bigger than your hips, spine, or wrists. You start wondering about everyday things that never seemed connected before. Can osteoporosis affect teeth? Could it change the way your dentures fit, the way your gums feel, or whether dental implants are still possible?
Those are smart questions.
Many people in Chattanooga and Cleveland are surprised to learn that bone health and oral health are closely linked. Your teeth don’t sit in isolation. They’re supported by jawbone, gum tissue, and the structures around them. When bone becomes weaker in one part of the body, it can affect what happens in the mouth too.
If you’re searching for a dentist near me because you’ve noticed loose teeth, sore gums, changes in your bite, or concerns about tooth extraction or dental implants, it helps to understand the full picture first. A careful dental exam can reveal signs that deserve attention, and a clear treatment plan can help you move forward without guessing.
Your Trusted Dentist for Complete Health in Chattanooga and Cleveland
A common story goes like this. A woman in her fifties or sixties gets told she has low bone density or osteoporosis. She leaves the appointment thinking about fractures, posture, and medication. A few days later, another thought creeps in. “What about my teeth?”
That question matters.
Your mouth is part of your overall health, not a separate system. If you’ve noticed a tooth feeling less stable, a denture fitting differently, or gums that seem to be changing, it’s reasonable to ask whether bone loss could be involved. Many patients in Chattanooga, TN, and Cleveland, TN ask that same question when they come in for cleaning and exams, restorative dentistry, or a new patient exam.
Why this concern is so common
Osteoporosis weakens bone. Your jaw contains the bone that supports your teeth, so it makes sense that changes there can affect your smile.
For many people, the hardest part isn’t the diagnosis itself. It’s not knowing what to do next.
A good dental visit should do more than check for cavities. It should connect the dots between your medical history, your symptoms, and the condition of your teeth and jaw.
That’s especially important if you’re considering treatment such as tooth extraction, periodontal care, or dental implants near me. Bone quality can shape which options are safest and most predictable.
What patients usually want to know
Most concerns fall into a few practical categories:
- Will osteoporosis make me lose teeth
- Can I still get dental implants
- Are my medications important to tell my dentist about
- Could changes in my gums or denture fit be related to bone loss
- What should I do now if I live in Cleveland or Chattanooga and need care
These are not overreactions. They’re the right questions.
A thoughtful dentist in Cleveland, TN or Chattanooga, TN should look at your oral health in the context of your full health picture. That means listening carefully, reviewing medications, taking dental x-rays when needed, and coordinating with your physician if treatment planning calls for it.
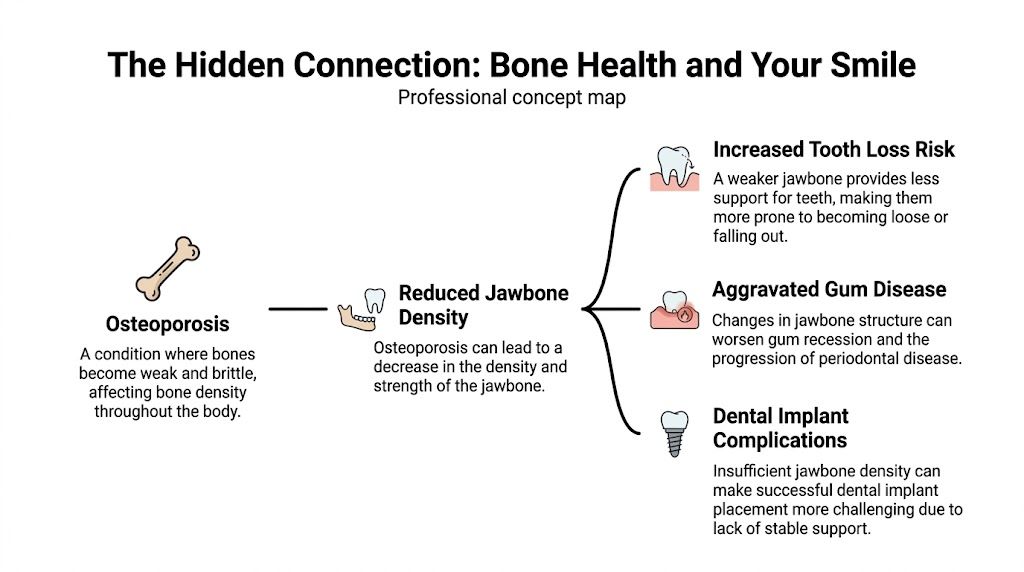
The Hidden Connection Between Bone Health and Your Smile
Osteoporosis means bones become weaker and less dense. Osteoporosis often brings to mind the hip or spine, but the jawbone can be affected too.
The easiest way to understand it is to think of your jawbone as the foundation of a house. Your teeth are the parts you can see above ground. If the foundation becomes weaker, the structure on top becomes less stable.
Why the jaw matters so much
Teeth are not only in the gums. They’re anchored in bone called the alveolar process, which helps hold the roots in place.
When that bone loses density, it may not support teeth as securely as it once did. That can lead to mobility, shifting, and in some cases tooth loss. Research found that women with osteoporosis are three times more likely to experience loose teeth and tooth loss than women without osteoporosis, according to this clinical review on osteoporosis and oral findings.
It’s not only about the tooth itself
People often get confused: Osteoporosis doesn’t usually damage the visible enamel in the way a cavity does. Instead, it affects the support system around the tooth.
That support system includes:
- Jawbone support that holds roots in place
- Gum attachment that helps seal and protect the area
- Periodontal structures that keep teeth stable during chewing
If the bone becomes thinner or weaker, normal biting forces may become harder for the body to manage. A tooth can start to feel “different” long before it falls out.
Gum disease can add to the problem
Osteoporosis and gum disease can interact in ways that make both more concerning. If the jawbone is already vulnerable, inflammation from periodontal disease can make support around the teeth even weaker.
If you want a simple overview of that broader body-mouth relationship, this article on the surprising link between gum disease and your overall health is a useful companion read.
Practical rule: If you have osteoporosis and your gums bleed, recede, or feel tender, don’t assume it’s minor. That combination deserves a closer look.
How dentists may spot changes early
Dental care plays an important role because dentists can often see jawbone changes on dental x-rays before a patient notices obvious symptoms. A routine exam may reveal signs such as reduced bone support, changes around tooth roots, or patterns that suggest a medical follow-up would be wise.
That doesn’t mean every dental change equals osteoporosis. It does mean your dentist can be part of early detection.
For patients in Chattanooga and Cleveland, that partnership matters. A local dental team can monitor your mouth, your physician can monitor your overall bone health, and together they can help you make informed decisions instead of waiting for a problem to get worse.
Oral Health Warning Signs of Systemic Bone Loss
Sometimes the first clues aren’t dramatic. They’re subtle changes you notice while brushing, chewing, or putting in a denture.
A tooth may feel slightly loose. Your gums may seem lower than they used to be. A partial or full denture may not sit the same way it once did. These aren’t details to ignore.

Signs you might notice at home
Here are some of the oral changes that can point to shrinking or weakening support around the teeth:
- Loose teeth that don’t feel as stable when you bite
- Receding gums that make teeth look longer
- Changes in denture fit that happen without a clear reason
- Jaw discomfort or pressure when chewing
- More missing teeth over time than you expected
A commonly missed detail is denture fit. Dentures rest on the shape of the jaw. If the bone underneath changes, the appliance may start rocking, rubbing, or feeling off.
When tooth loss becomes a clue
Research described in this overview of osteoporosis and dental effects reported that postmenopausal women with osteoporosis had a mean tooth loss of 5.4 teeth, compared with 1.09 teeth in women with normal bone density. The same review noted that losing three or more teeth was associated with significantly greater odds of osteoporosis.
That doesn’t mean every person with missing teeth has osteoporosis. Cavities, injuries, gum disease, and older dental work can all play a role. It does mean a pattern of tooth loss can be an important health clue.
Why gums can appear to recede
People often assume gum recession is only a gum problem. Sometimes the underlying bone is changing too.
When bone support shrinks, the soft tissue around it can change shape. Teeth may appear longer, spaces may open, and food may catch more easily.
If you want a helpful primer on that process, this page on bone loss in teeth explains the basics in plain language.
If your mouth feels different, trust that observation. You don’t need severe pain for a change to be worth evaluating.
What to do next
The next step isn’t self-diagnosis. It’s a proper exam.
A new patient exam with updated dental x-rays can help sort out whether you’re dealing with gum disease, bite trauma, age-related wear, bone loss, or a combination of issues. If you’re looking for a dentist in Cleveland, TN or Chattanooga, TN because something has changed in your mouth, that kind of exam gives you real answers instead of online guesswork.
How Osteoporosis Impacts Your Dental Treatment Plan
Once bone density becomes part of the picture, dental treatment planning gets more personalized. That’s not bad news. It just means your dentist has to think carefully about support, healing, and long-term stability.
Some procedures depend heavily on bone. Others can be adjusted to work around limitations.

Dental implants and bone support
A dental implant needs enough healthy bone to hold it firmly while it integrates with the jaw. If the bone is too thin or too weak, the plan may need to change.
That doesn’t automatically rule implants out. It does mean the evaluation matters more.
Research summarized by Eriks Dental Group on osteoporosis and implant success notes that low bone mineral density can interfere with osseointegration, with some meta-analyses reporting implant success dropping from over 98% in healthy bone to 70 to 85% in patients with severe bone loss. That’s why advanced imaging matters before treatment begins.
Why imaging changes the conversation
A standard exam tells part of the story. Detailed imaging can reveal the shape and volume of available bone, show nearby anatomy, and help your dentist judge whether an implant, bridge, crown, or another restoration makes the most sense.
For some patients, the most practical path is to preserve existing teeth through periodontal therapy or restorative dentistry. For others, implants are still possible with extra preparation.
If you’re reading about grafting because your dentist mentioned it, this explainer on understanding bone grafting gives a clear overview of why added bone support may be recommended before implant placement.
Tooth extraction may require more planning
Tooth extraction can also be more nuanced in someone with osteoporosis, especially if healing may be slower or medication is part of the picture.
That doesn’t mean you should avoid needed treatment. A problematic tooth can create infection, pain, and more bone loss if left untreated.
What changes is the level of planning. Your dentist may want:
- A more detailed medical history before scheduling
- Updated x-rays or 3D imaging to assess bone support
- Coordination with your physician if you take osteoporosis medication
- A different replacement plan after extraction, depending on bone quality
Later home care matters too. Patients often do better when they understand how to protect the area and maintain any implant or restoration over time. This guide on how to care for dental implants is a useful starting point for that phase.
A short video can also help make implant planning easier to visualize.
Other treatment options may fit better
Some patients hear “bone loss” and assume their options are gone. Usually, that’s not the case.
Depending on your needs, your dentist may talk with you about:
| Situation | Possible approach |
|---|---|
| A weakened tooth that can still be saved | Restorative dentistry such as a crown |
| A missing tooth with limited bone | Bridge options or other replacement planning |
| Several compromised teeth | A phased plan that protects function first |
| Significant bone limitations | Alternative implant strategies, including smaller implant designs in appropriate cases |
Winn Smiles offers mini implants for some patients with less bone density. Whether that’s appropriate depends on your exam, your goals, and the condition of the surrounding tissue.
The key point is simple. Osteoporosis changes the planning process. It doesn’t end the conversation.
Navigating Osteoporosis Medications and Your Dental Care
For many patients, the most stressful part of this topic isn’t bone loss itself. It’s medication.
You may have heard warnings about certain osteoporosis drugs and dental procedures. That can sound alarming, especially if you already need a tooth extraction or other invasive care. The better approach is to replace fear with clear communication.

Why your medication list matters
Some medications used to treat osteoporosis affect how bone breaks down and rebuilds. That’s helpful for protecting skeletal health, but it can change how the jaw heals after certain dental procedures.
One concern is MRONJ, short for medication-related osteonecrosis of the jaw. In simple terms, it refers to a situation where an area of jawbone doesn’t heal normally after an invasive procedure.
The risk is not the same for every person or every medication. According to this discussion of osteoporosis drugs and oral health, the risk of MRONJ is low for oral bisphosphonates, at around 1 to 10 cases per 100,000 patient-years, and can be higher with IV forms. The same source notes that a possible drug holiday before an extraction may be discussed between your dentist and physician when appropriate in this review of jaw risks and osteoporosis treatment.
What your dentist needs to know
Bring a complete medication list. Include osteoporosis drugs, infusion history, supplements, and the name of the doctor managing your bone health.
That information can affect:
- Whether treatment should happen now or later
- Whether your physician should be contacted first
- How an extraction or surgical procedure is planned
- What healing precautions make sense afterward
Medication rule: Never stop an osteoporosis medication on your own because of something you read online. That decision belongs to you, your physician, and your dentist together.
What a drug holiday means
This phrase confuses a lot of people. A drug holiday is not a casual break you decide to take yourself.
It refers to a medically supervised pause that may be considered before certain invasive procedures. Whether it’s appropriate depends on the drug, your health history, fracture risk, and your physician’s judgment.
Sometimes a pause is recommended. Sometimes it isn’t. The right answer is individualized.
If you need emergency dental care
Don’t hide your medications because you’re worried treatment will be delayed. That only makes emergency care less safe.
If you need an emergency dentist for swelling, pain, or a broken tooth, tell the dental team about your osteoporosis diagnosis and medications right away. Even when urgent treatment is necessary, your providers can make better decisions when they have the full picture.
Remember this: Having osteoporosis or taking treatment for it does not mean dental care is off-limits. It means your care should be deliberate, coordinated, and well communicated.
Proactive Steps for Protecting Your Smile and Bones
The most helpful mindset is partnership. You, your dentist, and your physician each handle a different part of the same problem.
That shared approach often works better than trying to treat your mouth and your bones as unrelated issues. Small habits matter. So does routine professional care.
Daily habits that support both systems
A few basics do double duty for oral health and bone health:
- Stay consistent with home care so plaque and gum inflammation don’t get a foothold
- Eat with bone support in mind and follow your physician’s guidance on calcium and vitamin D
- Keep follow-up appointments instead of waiting for discomfort
- Tell all providers about changes in medications, symptoms, or planned procedures
If your jaw support is already vulnerable, preventing gum disease becomes even more important. Inflamed gums and irritated periodontal tissue can make an already fragile support system work harder.
Why routine dental visits matter more here
When someone has osteoporosis, regular cleaning and exams aren’t just about polishing teeth. They create a timeline.
Your dental team can compare x-rays, examine changes in gum levels, monitor loose areas, and catch patterns before they become crises. That’s useful whether you need preventive care, restorative dentistry, cosmetic dentistry, or help deciding if a missing tooth should be replaced.
Your mouth usually changes gradually. Regular exams help your dentist notice those small shifts before they turn into major treatment decisions.
Keep the conversation connected
Many patients divide their care into separate boxes. The physician handles bones. The dentist handles teeth. The problem is that your body doesn’t work that way.
Use each appointment to update the other side. If your physician changes medication, tell your dentist. If your dentist sees changes on dental x-rays or notices unusual tooth mobility, share that with your medical team.
A simple checklist can help:
| Tell your physician | Tell your dentist |
|---|---|
| New tooth loss | New osteoporosis medication |
| Ongoing gum problems | Infusion or injection history |
| Planned extraction or implant treatment | Bone density diagnosis |
| Changes in chewing or jaw comfort | Changes in denture fit |
The goal isn’t to make you anxious. It’s to help you stay ahead of problems.
For families in Chattanooga and Cleveland, the strongest plan is usually the least dramatic one. Routine care, good communication, and prompt attention when something feels off.
Your Partner in Health What to Expect at Winn Smiles
When a patient with osteoporosis walks into a dental office, they shouldn’t feel rushed or brushed aside. They should feel heard.
That starts with the first conversation. If you’re looking for a dentist near me in Chattanooga or Cleveland because you’re concerned about bone loss, implants, loose teeth, or a possible extraction, your visit should begin with a full health review, not just a quick look at one tooth.
A first visit that connects the dots
A new patient exam typically works best when it includes time to talk through:
- Your osteoporosis diagnosis
- Your medications and supplements
- Changes in your teeth, gums, or dentures
- Any pain, mobility, or chewing concerns
- Whether you’re considering implants, crowns, or other restorative care
That history matters because it guides the rest of the visit. A loose tooth means something different in a person with healthy bone than it does in someone with known bone loss.
Imaging that helps with real decisions
Digital dental x-rays can help show the condition of the bone around your teeth. In some cases, 3D imaging gives a more complete picture when treatment planning involves an extraction, implant, or more advanced restorative work.
Patients often feel calmer once they can see what the dentist is describing. It turns an abstract fear into a visible, understandable problem with a plan attached to it.
You deserve to know not only what’s happening, but why your dentist is recommending a certain path.
Comfort matters too
Bone loss concerns often come with a second layer of stress. Some patients are worried about pain. Others are embarrassed that they waited. Some are anxious because they’ve had difficult dental experiences before.
A comfort-focused office can make a real difference. Clear explanations, sedation options for appropriate cases, and a team that moves at a steady pace can make care feel manageable again. That matters whether you’re coming in for a routine exam, periodontal treatment, same-day crowns, or emergency dentistry.
Local care for Chattanooga and Cleveland patients
Practical convenience matters when you’re juggling physician appointments, medication questions, and dental treatment at the same time. Having access to local care in Chattanooga, TN and Cleveland, TN makes follow-up easier, especially when your treatment needs to be coordinated over time rather than handled in one rushed visit.
For many patients, the biggest relief is simple. They find out they don’t have to solve this alone.
A good dental office won’t just say “you have bone loss” and send you home worried. It will explain what the findings mean, what can be watched, what should be treated, and when your physician needs to be involved. That kind of care feels less like damage control and more like a plan.
Frequently Asked Questions About Osteoporosis and Dental Care
Can improving my osteoporosis reverse dental problems
Not always. It may help protect future bone health, but existing tooth loss, gum recession, or structural changes in the jaw often still need dental treatment. The goal is usually to prevent progression and manage the problems already present.
Are dental implants still possible if I have osteoporosis
Sometimes, yes. It depends on your bone support, medical history, and healing risk. Some patients may still be candidates for implants, while others may do better with bridges or other restorative options.
If I have severe bone loss, what alternatives exist besides implants
That depends on where the missing teeth are and how much support remains. Crowns, bridges, partial dentures, full dentures, and phased restorative treatment can all be part of the discussion. Your exam determines which path is realistic.
Should I tell my dentist even if my osteoporosis medication seems unrelated to my mouth
Yes. Always. Medications used for bone health can affect how your jaw responds to certain procedures, especially extractions and other invasive treatment. Your dental team needs that information before planning care.
How often should I get dental x-rays if I have osteoporosis
There isn’t one schedule that fits everyone. Your dentist will recommend x-rays based on your symptoms, treatment history, gum health, and risk factors. If you’ve noticed changes like loose teeth or shifting dentures, updated imaging may be important sooner.
Can a dentist be the first person to notice a problem
Yes. Dental exams and x-rays can reveal changes in the jawbone or tooth support that deserve a closer medical look. A dentist can’t diagnose every bone condition from a routine exam alone, but they may notice warning signs that should not be ignored.
Does osteoporosis cause cavities
Not directly in the way sugar and bacteria do. Cavities affect the hard outer structure of the tooth. Osteoporosis affects the bone support around teeth, which is a different issue. Some patients have both concerns at the same time.
What should I do if I’m worried right now
Schedule an exam. If you live in Chattanooga or Cleveland and you’ve noticed loose teeth, gum changes, denture fit problems, or questions about dental implants near me, getting evaluated is the clearest next step. A personalized exam is much more useful than trying to connect every symptom on your own.
If you’re concerned that osteoporosis may be affecting your teeth, gums, or treatment options, schedule a visit with Winn Smiles. A careful exam, dental x-rays, and a conversation about your medical history can help you understand what’s happening and what to do next in Chattanooga or Cleveland.



